Ice Hockey COVID Outbreaks
Air Date: Week of November 6, 2020

Getting a flu shot may be particularly important this year, as coronavirus stresses medical resources. (Photo: Phillip Jeffrey, Flickr, CC BY-NC-ND 2.0)
With the onset of winter in the Northern Hemisphere come new concerns about what effect the reduction of sunlight and increased time spent indoors might have on coronavirus spread. Several outbreaks have occurred in connection with recreational and youth hockey, and researchers are rushing to pin down the role of air temperature and humidity in creating optimal conditions for contagion. For some advice about getting through winter safely, Host Steve Curwood caught up with pediatrician Aaron Bernstein, the interim director of Harvard’s Center for Climate, Health and the Global Environment.
Transcript
CURWOOD: The Covid 19 pandemic is accelerating in the northern hemisphere as colder weather settles in. Hospitals and health care workers are struggling in many communities, especially in the US where the daily tally of new cases is spiking at record levels. The trend is expected to continue as more activities shift indoors. There is much that science still has to learn about Covid-19, such as why indoor recreational ice hockey has been associated with outbreaks in several states, not just in the north but also in Florida, where about a dozen people got Covid 19 after a game at a hockey rink in Tampa Bay. For some advice for getting through winter safely we turn now to Dr. Aaron Bernstein, he’s Pediatrician at Boston Children’s Hospital and interim director of Harvard’s Center for Climate, Health and the Global Environment. Welcome back to Living on Earth, Ari!
BERNSTEIN: Great to be with you, Steve.
CURWOOD: So we're seeing coronavirus outbreaks in connection with indoor ice hockey practices to a greater extent than what's been seen in other sports and activities. Walk us through in basic terms, what about the virus might make it more dangerous for these cold weather sports and as the colder weather approaches?
BERNSTEIN: Well, I think we're still digging into what's going on in the skating rinks. But the best clues we have right now is that transmission may not be happening as much on the ice, but may be happening off the ice in locker rooms or on the bench when people may take off protective gear or sit too close with each other. We don't really know. But it's pretty clear that since there have been outbreaks in multiple states associated with hockey playing, that there is something about it that matters. But we mostly see in in other indoor settings transmission happening when you've got people sticking around each other for long periods of time. And so that makes locker rooms, for example, a prime suspect.

Recreational hockey seems to be a high-risk activity for coronavirus, but the exact reason is still under investigation. (Photo: Pointnshoot, Flickr, CC by 2.0)
CURWOOD: How fair is it to assume that the locker rooms are also really pretty cold adjacent to the ice and in the building that's trying to keep the ice there?
BERNSTEIN: We do know a couple of things. I mean, what's clear is that sunlight is really good at inactivating the virus. So, you know, ice skating rinks are not in a lot of sunlight, whether it's the ice or the locker room, that's true, obviously, of any indoor environment. So the ultraviolet piece seems to be a pretty strong signal in terms of temperature, and humidity, it gets kind of messy. And that's one of the reasons why the winter people are concerned because particularly here in the Northern Hemisphere, there's a lot less ultraviolet radiation hitting us from the sun.
CURWOOD: So as we move into winter, of course, historically, the influenza virus seems to do much better in the winter. What parallels can we draw between the influenza virus and the novel coronavirus in terms of transmission in this cold part of the year?
BERNSTEIN: Well, I think the big deal in winter transmission of viruses that are transmitted by you know, coughs and sneezes, and the droplets they can leave on surfaces, is that people tend to gather indoors a lot more in the winter. That's a risk factor for any of these viruses. And so when I think about the winter, I do think we need to pay close attention to places where we're asking people to congregate, and being careful about the appropriate precautions to ensure that we're not having, you know, unnecessary spread. I mean, it's, we're breaking records in transmission as we speak and there's a great risk that this virus can spread through the winter, the idea has been floated that herd immunity will protect this is reckless and dangerous. And we can do a tremendous amount even now, to reduce, we can't eliminate at this point, but we can reduce the amount of spread through the basic measures that leaders in public health have been talking about for a long time now.
CURWOOD: What's the best thinking about how communities can protect their most vulnerable members, during this time of rising numbers of these cases, rising exposure, apparently better conditions for the virus?
BERNSTEIN: Yeah, you know, it probably is sounding completely boring and beating a dead horse. But it's the same dull stuff that folks have been talking about for a long time, it's wearing a mask, it's washing your hands, it's keeping physical distance. And those measures can have a dramatic effect upon the spread of disease. And you know, there are people anguishing a lot right now about what's safe in terms of, you know, should we go to place a, b, or c, and that is entirely dependent upon the spread of the disease in the community. If you're living in a place, you know, right now, we have tremendous case burdens in the upper Midwest, in particular, you know, the risks of doing the things that people are thinking about doing are much higher when you have higher case counts in the community, even with those protective measures. But you know, I think a lot of people, including folks like Tony Fauci, and other public health leaders have strongly advised people to not gather in person, because the risks are growing so great, because the reality is that we have more cases today in the country than almost any other time. And the signs are this winter, it may not get better quickly.
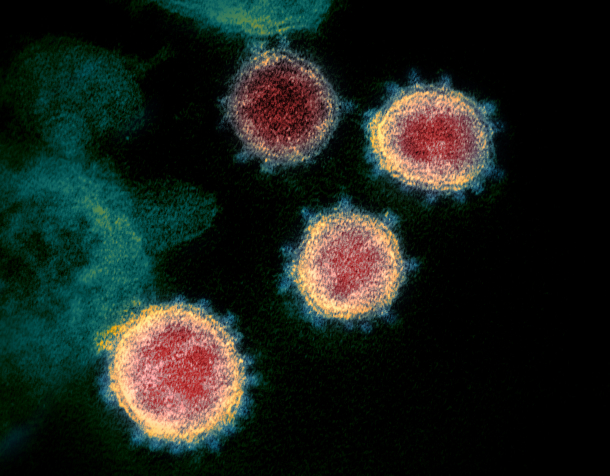
The novel coronavirus seems to degrade quickly when exposed to UV light, and seems to be more transmissible at particular levels of heat and humidity. (Photo: NIAID-RML, Wikimedia Commons, CC by 2.0)
CURWOOD: So know, to what extent to things change if a vaccine becomes widely available in the next few months.
BERNSTEIN: Yeah, well, I think the first thing to acknowledge is that we hopefully will have an effective vaccine in the next few months. But it's clear that that most people will not have access to that well into 2021. And so we can't really bank on that as a way to get us out of this mess in the next few months of this year. And probably not in the first few months of the next year. We also have an issue in which there are many people in the country who don't want to vaccinate. And that's, you know, a real challenge because again, the risk isn't just to the individuals who don't vaccinate, it's to the people who live in their communities. And, you know, it's as a pediatrician, you know, we deal with this concern all the time, which was we don't have many, but there are some families who do not want to vaccinate their children or don't want to vaccinate on the usual schedule or want vaccine one versus vaccine two. And these are obviously concerns for the child. We don't give these vaccines because the diseases aren't a problem we give them because the diseases are a big problem. But it's very much a concern for the people they live with. I have more stories than I would ever want to know about a family who did not vaccinate, their children got sick and their children were okay, but they infected someone else's children. And those children were not okay. And who really wants to live with that sense of, you know, grief, that we have a vaccine for preventable diseases and that, you know, by not getting ourselves vaccinated, we put other people at risk who are, you know, don't do as well. And I think that's very much the case with Coronavirus. You know, we see now high rates of transmission among people who are younger, who tend to be okay. But those infections don't limit themselves to geographic borders, or political parties or religions or anything. So we just have to remember that part of our action here is not just for ourselves, it's for the people who live in our country and in, you know, our communities. And beyond that, you know, it's making sure that people get their flu vaccines, right. So people don't see those two connected to they're actually very much connected. So we're going to have a flu epidemic this year, like we do every year, we can hope that it is not a bad flu year. We don't know yet. But it's gonna come and there's a vaccine. And the reason they're connected is that we know we're going to have a tremendous burden of coronavirus cases we already see in many states hospital beds, essentially being at max capacity. Well, that's what happens in a bad flu season. So if you take the current coronavirus season, and you add to it even a mild flu season, there are no hospital beds for people to go into. We can do a lot more now today than we could at the start of this virus to keep people who get sick enough to be hospitalized from getting severely ill. But if we're picking and choosing hospital beds and don't have hospital beds, it makes our lives as healthcare providers majorly more difficult. So I you know, there are a lot of people who don't want to get vaccinated for the flu because they think it's not that bad, or they think the flu vaccine doesn't work. And neither of those things are true. And so this is really an issue of protecting healthcare resources, not to mention protecting yourself and your family. And again, the flu is a major factor in severe illness and people who are older, so in one of the populations that's really at risk from coronavirus are also really at risk for their flu.

Dr. Aaron Bernstein works as a pediatrician, but also coordinates research on the intersection of the climate, air pollution, and human health. (Photo: Courtesy of Aaron Bernstein)
And so, you know, I'm, you know, I'm not over 65 and I have to get vaccinated, so I work in health care. But even if I didn't, I would recognize that if I want to protect my family, I should be getting vaccinated against the flu to protect people who are older than me, my family members who may have cancer, my family members who may be pregnant. You know, think about it. If you have a family member who's pregnant, they often need to go to a hospital. Do you really want them to go to a hospital in which the hospital is overwhelmed with preventable influenza infections? No. Obviously. So that's how these things tie together pretty quickly.
CURWOOD: Ari Bernstein is a pediatrician at Children's Hospital in Boston and directs the Climate Health Program at the Harvard TH Chan School of Public Health. Dr. Bernstein, thanks so much for taking the time with us today.
BERNSTEIN: Thanks for having me, Steve.
Links
Read the CDC report on an outbreak at a Tampa Bay Hockey game
Read more about Massachusetts' decision to shut down youth hockey until more data could be gathered
Learn why influenza virus cases surge in winter
Living on Earth wants to hear from you!
Living on Earth
62 Calef Highway, Suite 212
Lee, NH 03861
Telephone: 617-287-4121
E-mail: comments@loe.org
Newsletter [Click here]
Donate to Living on Earth!
Living on Earth is an independent media program and relies entirely on contributions from listeners and institutions supporting public service. Please donate now to preserve an independent environmental voice.
NewsletterLiving on Earth offers a weekly delivery of the show's rundown to your mailbox. Sign up for our newsletter today!
 Sailors For The Sea: Be the change you want to sea.
Sailors For The Sea: Be the change you want to sea.
 The Grantham Foundation for the Protection of the Environment: Committed to protecting and improving the health of the global environment.
The Grantham Foundation for the Protection of the Environment: Committed to protecting and improving the health of the global environment.
 Contribute to Living on Earth and receive, as our gift to you, an archival print of one of Mark Seth Lender's extraordinary wildlife photographs. Follow the link to see Mark's current collection of photographs.
Contribute to Living on Earth and receive, as our gift to you, an archival print of one of Mark Seth Lender's extraordinary wildlife photographs. Follow the link to see Mark's current collection of photographs.
 Buy a signed copy of Mark Seth Lender's book Smeagull the Seagull & support Living on Earth
Buy a signed copy of Mark Seth Lender's book Smeagull the Seagull & support Living on Earth